Platelets are small blood cells whose function is to cause the blood to clot when there is an injury and prevent heavy bleeding. Platelets have large quantities of growth factors, which, when injected, enable the patient to begin a process of growth and regeneration of cartilage, collagen tissue, muscle, skin and even hair. In comparison to prolotherapy, a technique that incites the production of growth factors, platelets have already these growth factors ready to act. Over 15,700 articles, including several thousand randomised controlled trials, have been published in ‘Pubmed’ alone, which reflects the growing interest in this field. In order to achieve good long-term results, ideally the whole functional unit around the injured area should be treated and not just the single structure that is damaged. Very few therapists do this.
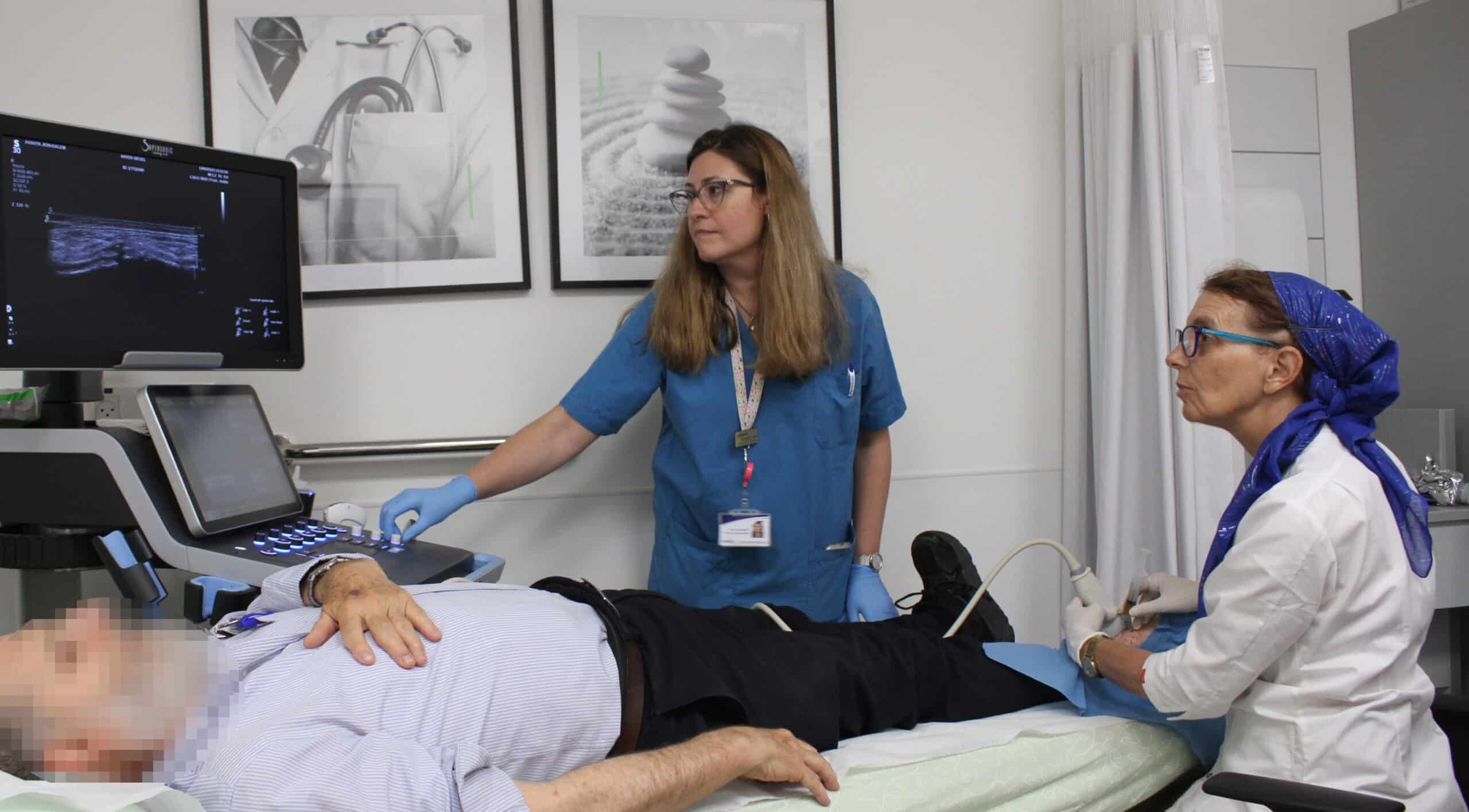
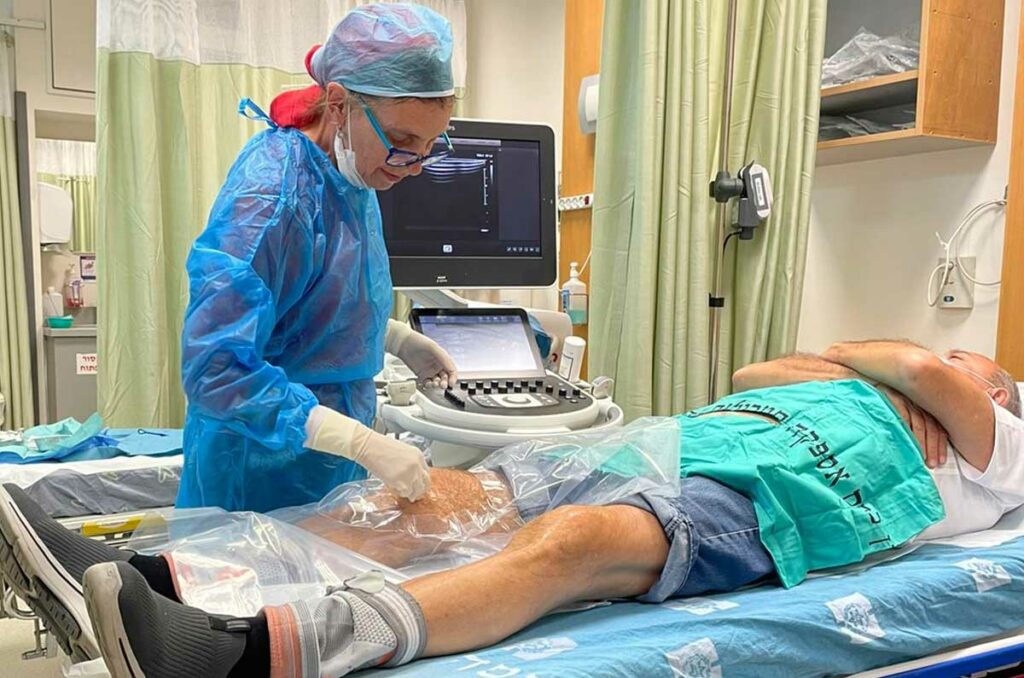
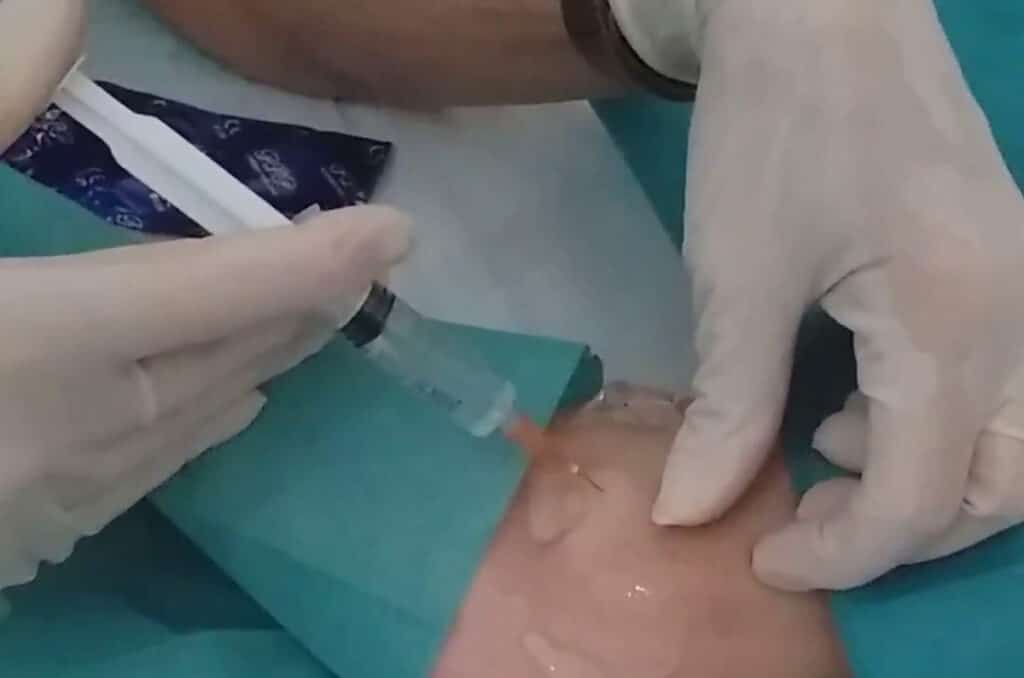
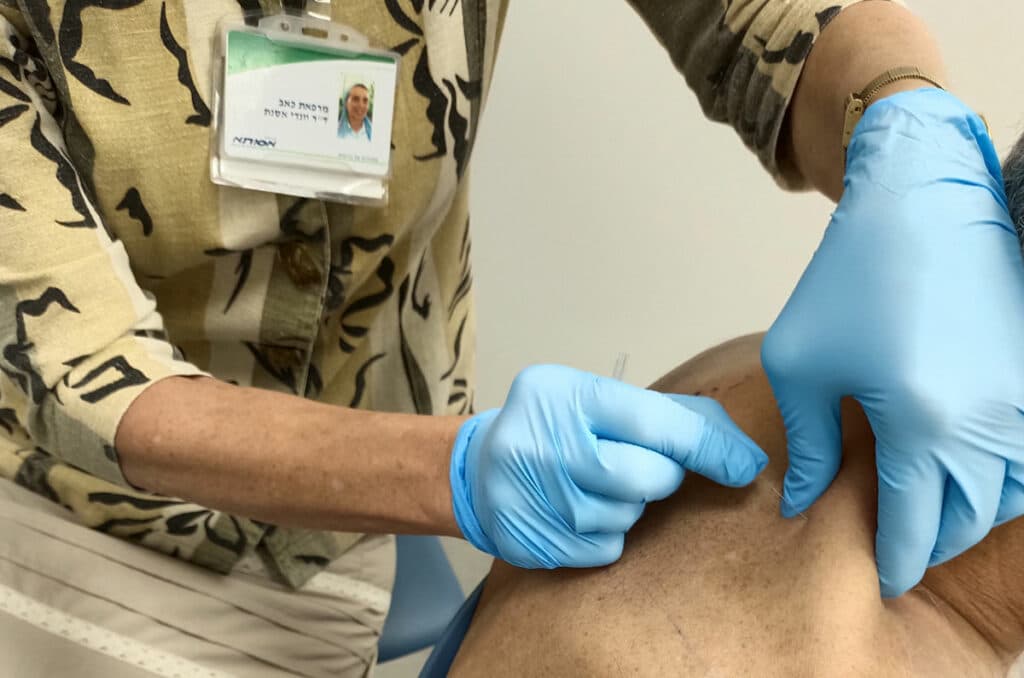
What does PRP treatment entail? First blood is withdrawn from the patient in a sterile fashion, and this blood is separated into different components while being spun in a centrifuge. The platelets are concentrated into a smaller volume of plasma, and injected into the damaged tissues together with important plasma proteins present in the plasma. The platelet-poor plasma is usually discarded (though sometimes the proteins in this part of the blood are also useful for treating certain conditions) together with the red blood cells.
Most physicians who use PRP use certain disposable kits to prepare the final product, a factor that adds significant cost to the treatment.
Different pathologies treated by PRP:
- Partial tendon and ligament tears
- Osteoarthritis
- Localised nerve damage
- Treatment of chronic low back pain and facet joint arthropathy
- Bone or ligament grafts
- Dental implants
- Aesthetic medicine- treatment of balding, facial treatments.
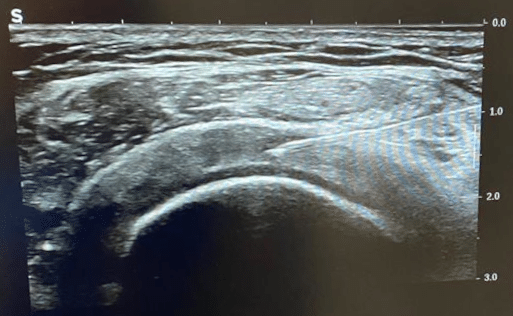
In our clinic, treatment is targeted at musculoskeletal pathologies and localised nerve damage. There are various types of PRP. Some PRP treatments focus on the concentration of growth factors, while others on the anti-inflammatory components of PRP. In addition, there are variations depending on the dose of added anti-coagulant and which one (if used at all), whether calcium chloride which hastens the blood clot is added, whether the white blood cells are concentrated or not and the speed of centrifugation. The latter has an impact on the survival of the platelets. There are advantages and disadvantages to each of these variations.
Platelet-Rich Fibrinogen (PRF)
PRF is a special PRP version which does not use any anticoagulant which would prevent clotting. The blood is centrifuged, the platelets are aspirated and then injected almost immediately. Theoretically, as soon as the platelets clot within the body, they release the growth factors, and this becomes very effective. The fact that there is a small clot in the area injected ensures that there is a scaffold which holds the platelets and the growth factors in place for their action to take place. Other methods which lack a scaffold have no way of keeping the platelets and growth factors in place to act. PRF is especially effective for the treatment of osteoarthritis and partial tendon and ligament tears.